Link ex Steudel (1824)
What is Epidermophyton?
Epidermophyton is a genus of filamentous fungus belonging to an ecological group of pathogenic fungi called dermatophytes. There exist around forty species of dermatophytes, classified into four genera Epidermophyton, Microsporum, Trichophyton, and Chrysosporium.
Certain dermatophytes have been found to produce sexual states, and are classified into the genus Arthroderma. All dermatophytes are characterized by their ability to grow in dead tissues of skin, nails, and hair, feeding on protein keratin. The living tissues are not infected since dermatophytes are not able to grow at 37 °C (98.6 °F). However, products of their metabolism can cause inflammatory processes [1].
Eidermophyton species
The genus Epidermophyton comprises two species, distributed worldwide: E. floccosum and E. stockdaleae [2]. E. stockdaleae is found exclusively in soil and is considered non-pathogenic, while E. floccosum is associated with ringworm infections in humans. It is considered an anthropophilic (infects humans) species and is rarely isolated from dogs or other animals [2].
What are cultural and morphological characteristics of Epidermophyton?
Colonies of Epidermophyton on Sabouraud’s dextrose agar at 25–30 °C (77–86 °F) are slow-growing, greenish-brown, or khaki. They are characterized by a velvety surface, radial grooves, and a raised, folded center [2].
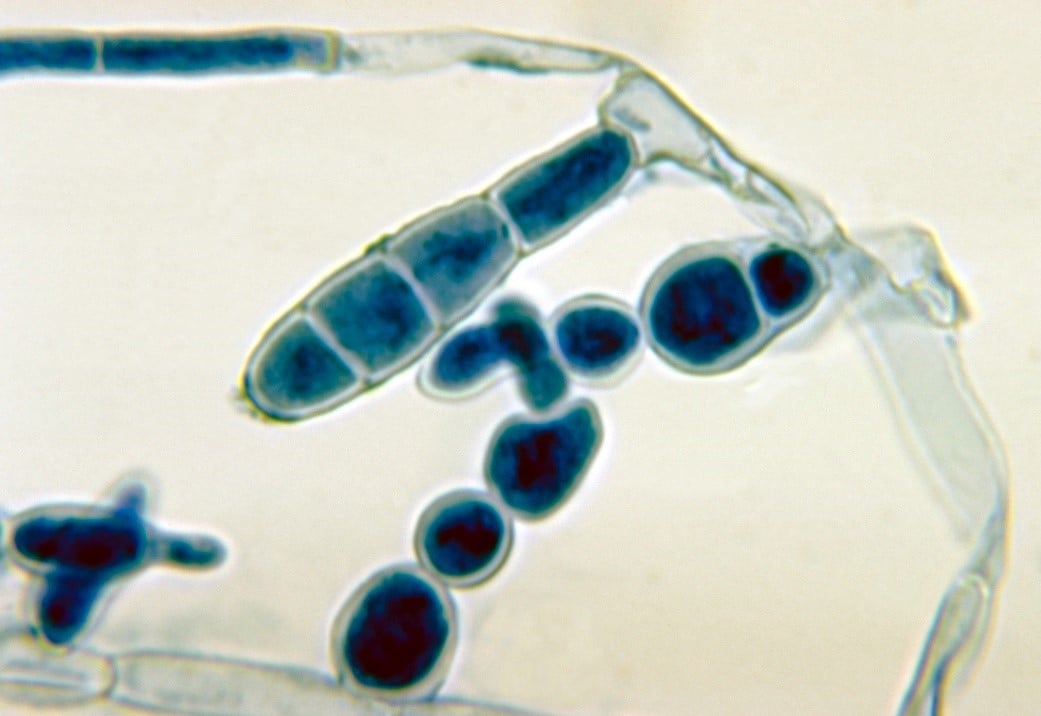
Microscopic morphology shows septate hyphae with large, smooth, asexual spores – macroconidia (Fig. 1). Epidermophyton spp. does not form microconidia. Macroconidia grow directly from their hyphae, occurring singly or in clusters. They can be thin or thick-walled, divided into 1-9 septa [2]. In a host tissue, E. floccosum produces numerous chlamydospores (arthrospores) by hyphal fragmentation [1, 2].
Chlamydospores are thick-walled and resistant to unfavorable conditions, providing longer viability in the environment compared to other propagules. They also act like the infectious agent, enabling transmission between the hosts or from the environment to the host [2].
What is Epidermophyton infection?
After transmission, chlamydospores of E. flocossum germinate in the skin epidermis without further penetration into the host tissue. Depending on the infected body part, E. flocossum can cause athlete’s foot (tinea pedis), body ringworm (tinea corporis), or jock itch (tinea cruris) when the groin and inner thighs are affected. Nail infection (onychomycosis) caused by E. floccosum has also been reported, while this fungus is not known to affect hair [2].
What are symptoms of Epidermophyton infection?
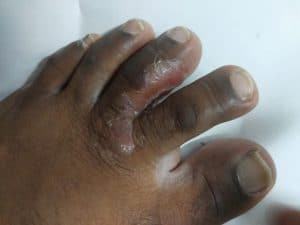
Athlete’s foot (tinea pedis) caused by E. floccosum is moccasin type, affecting the entire plantar surface and extending to the lateral foot (Fig. 2). The redness of the skin is mild, so the condition may be asymptomatic. A dry, hyperkeratotic scale with fissures may develop on one or both feet. If untreated, the disease can affect toenails [3].
Body ringworm (tinea corporis) is dermatophytosis of the smooth skin of the face (excluding the beard), trunk, and limbs. It is a very common disease, mostly prevalent in people living in tropical climates. Immunocompromised individuals, patients with systemic diseases, and people with outdoor occupations are especially prone to developing body ringworm. Being an anthropophilic pathogen, E. flocossum causes noninflammatory scaly plaques with an annular shape, with advancing scale and central healing. Lesions are usually itchy [3].
Jock itch (tinea cruris) caused by dermatophytes does not occur very often. Symptoms include a red and very itchy rash that affects the groin and inner thighs and may be shaped like a ring. Tinea cruris caused by E. floccosum is chronic and relatively noninflammatory infection. The disease is more likely to occur in men, usually affecting the fold near the scrotum as the first area. Infection can spread to the pubis, perineum, perianal area, and buttocks. Lesions may be symmetrical or asymmetrical, affecting one or both body sides [3].
Nail infection (onychomycosis or tinea unguium) caused by E. floccosum is not so common. The fungus invades the nail plate at the lateral nail groove and migrates. Following mild inflammation, frequently results in separation of the nail plate from the nail bed (onycholysis) and thickening of the nail. Due to secondary (bacterial or mold) infection, yellowish-brown discoloration might also be present [3].
How to treat Eidermophyton?
In the cases of athlete’s foot and jock itch, topical application of terbinafine, butenafine, itraonazole, voriconazole, and ketoconazole is recommended [3, 4]. In severe or chronic cases, oral antifungals may be necessary due to the reappearing of infection. Treatment by antibacterial may also be needed to prevent secondary infections [3].
Preventive measures are very important, considering wearing clean clothes and shoes, avoiding tight-fitting clothes, and avoiding sharing personal items such as clothing, brushes, or towels. Personal hygiene is also helpful in prevention. Since dermatophytes are very common in communal facilities such as bathing areas, changing rooms, as well as in domestic carpets [1], appropriate disinfection is mandatory. Spores of dermatophytes fungi are susceptible to benzalkonium chloride, 1% sodium hypochlorite, enilconazole, formaldehyde, iodophors, glutaraldehyde, and phenolic compounds. E. floccosum is particularly sensitive to benzylammonium bromide and ethoxyllauric alcohol, as well as to dihydrofarnesol [2].

Did you know?
Only 11% of tested bedrooms in Canada didn’t have any mold type present?! Find out more exciting mold stats and facts on our mold statistics page.
References
- Deacon, J. W. (2006). Fungal Biology. Blackwell Publishing Ltd. 4th Edition. pp. 324-327.
- Samanta, I. (2015). Veterinary Mycology. Springer, New Delhi, India. pp 29-32.
- Dismukes, W.E.; Pappas, P.G. and Sobel, J.D. (2003). Clinical Mycology. Oxford University Press, Oxford. pp 370-384.
- Pfaller, M. A. & Eayne, P. NCCLS (1998). Standards. National Comittee for Clinical Laboratory Reference method for broth dilution antifungal susceptibility testing of conidium-forming filamentous fungi: proposed standard.

Get Special Gift: Industry-Standard Mold Removal Guidelines
Download the industry-standard guidelines that Mold Busters use in their own mold removal services, including news, tips and special offers:

Written by:
Jelena Somborski
Mycologist
Mold Busters
Edited by:
Dusan Sadikovic
Mycologist – MSc, PhD
Mold Busters
